Preventive Healthcare
Varicose Veins in Leg: Symptoms, Causes, Diagnosis, and Treatment
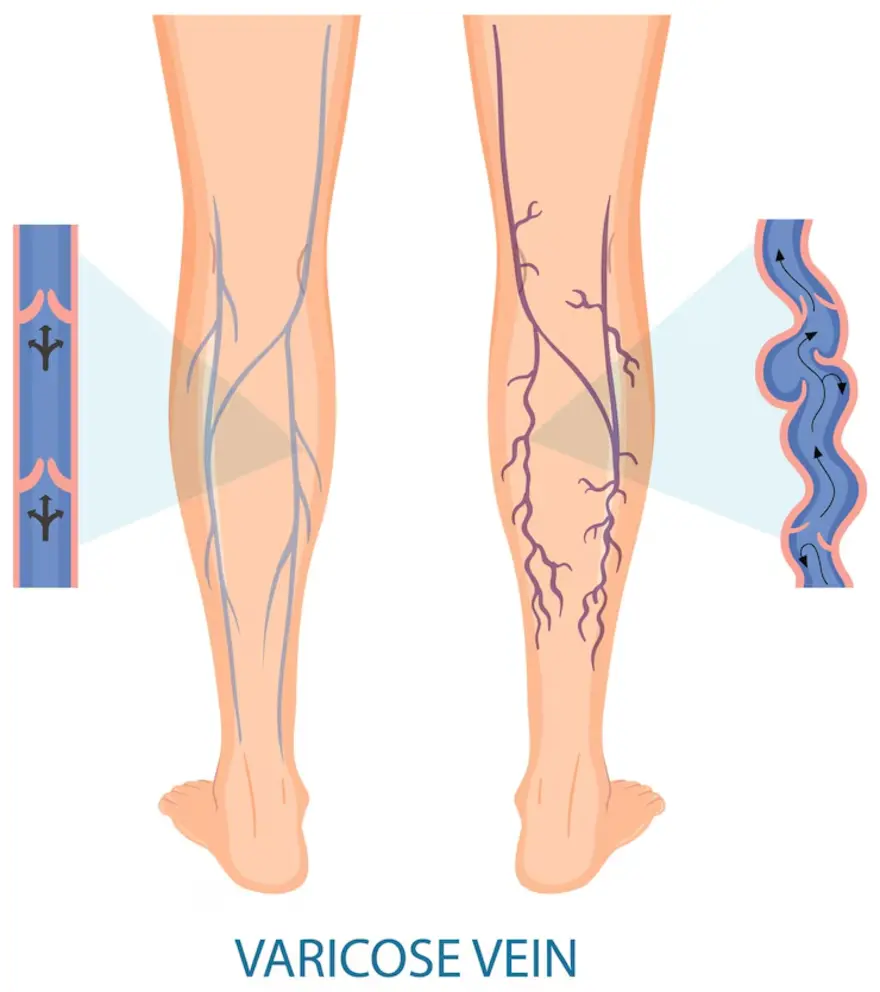
Table of Contents
- What are Varicose Veins?
- What is the Difference Between Varicose Veins and Spider Veins?
- Who is Likely to Get Varicose Veins?
- What are the Symptoms of Varicose Veins?
- Where Do Varicose Veins Usually Appear?
- What Causes Varicose Veins?
- What are the risk factors for varicose veins?
- How are Varicose Veins Diagnosed?
- What tests will be done to diagnose varicose veins?
- What is the Treatment for Varicose Veins?
- What are the Complications/Side Effects of the Treatment?
- How Can I Prevent Varicose Veins?
- What is the Outlook for People with Varicose Veins?
- What are the complications of varicose veins?
- Do varicose veins return after treatment?
- When to see a doctor?
- Conclusion
- FAQs
What are Varicose Veins?
Varicose veins are swollen and enlarged veins that typically occur in the legs. These veins, located close to the skin's surface, become varicose due to increased pressure, especially from prolonged standing or walking.
What is the Difference Between Varicose Veins and Spider Veins?
Varicose veins appear knobby and twisted and have a darkish-blue hue. Spider veins resemble varicose veins but are smaller and nearer to the skin's surface. They often exhibit red or blue colours and can resemble tree branches or spider webs commonly found on the legs or face.
Who is Likely to Get Varicose Veins?
Varicose veins are prevalent in women, particularly during hormonal shifts like pregnancy and menopause. Moreover, the risk escalates with age but can manifest in adulthood. Certain health conditions, including obesity, Deep Vein Thrombosis (DVT), and familial history, can increase susceptibility. Therefore, it is vital for individuals, especially those with predisposing factors, to maintain wellness and consult medical professionals if symptoms arise.
What are the Symptoms of Varicose Veins?
Common varicose vein symptoms that arise in people ara:
- Appearance: Veins appear bulging, twisted, and dark purple or blue
- Pain: Legs may feel achy, heavy, or sore, particularly behind the knees
- Swelling: Legs, ankles, or feet may swell
- Skin: Skin colour alterations around the veins, with potential brown discolourations, can be witnessed if untreated
- Other symptoms: These include itching, burning, throbbing, or muscle cramps around the veins, which often worsen at night
- Additional indicators: Sores on the legs, rash, dry, itchy, or thin skin over the affected vein
Where Do Varicose Veins Usually Appear?
Varicose veins, or varicosities, present as swollen, twisted veins, can appear throughout the body. Though these are frequently observed in the legs and feet, some common sites include:
- Calves
- Thighs
- Areas both behind and in front of the legs, especially near the ankles and feet
- During pregnancy, these may appear around the lower pelvic region, inner thigh, and buttocks.
What Causes Varicose Veins?
Varicose veins develop due to weakened or damaged vein walls and valves, which cause blood to pool and veins to become enlarged and twisted. Some other varicose vein causes include:
- Age: Vein elasticity diminishes with ageing
- Pregnancy: Varicose veins in pregnancy occur due to increased blood volume to support the baby's heightening pressure.
- Overweight: Excess weight adds strain to veins
- Prolonged sitting or standing: Extended periods in these positions may elevate risk
- Sedentary lifestyle: Lack of activity can contribute to heightened blood pressure
- Other factors: Smoking, oral contraceptives, hormone replacement therapy, leg injuries, chronic constipation, and insufficient vitamin K2 levels can also increase susceptibility to varicose veins.
What are the risk factors for varicose veins?
Varicose veins can develop due to a variety of risk factors that affect blood flow and vein strength. Age is a significant factor—over time, the valves in your veins may weaken, making it easier for blood to pool and cause vein enlargement.
Women are more susceptible to varicose veins, especially due to hormonal changes during pregnancy, menstruation, and menopause. A family history of varicose veins can also increase your chances, as genetic factors may influence vein health.
Obesity is another key contributor, as excess weight adds pressure on the veins, especially in the legs. Occupations or lifestyles that involve prolonged standing or sitting can impair proper circulation, leading to vein issues.
Additional varicose veins risk factors include pregnancy, smoking, and a sedentary lifestyle. Understanding these can guide you toward healthier habits and potential preventive steps.
How are Varicose Veins Diagnosed?
A healthcare professional can opt for any of the following varicose veins diagnosis:
- Physical examination: Your healthcare provider will assess your legs while standing to observe any swelling and examine the appearance of varicose veins.
- Medical history inquiry: Symptoms, family history, activity levels, and lifestyle are often discussed to understand potential risk factors.
- Imaging tests: A Duplex Ultrasound (DUS), a non-invasive method that utilises sound waves to evaluate blood flow in leg vessels, may be prescribed. This can help locate damaged valves contributing to varicose veins.
- Further investigation: If varicose veins cause pain, skin changes, or other complications, a referral to a vascular specialist may be warranted.
What tests will be done to diagnose varicose veins?
Diagnosing varicose veins typically involves a physical exam and non-invasive tests. Your doctor will visually inspect your legs and feel for any swelling or tenderness. They may also use a Doppler ultrasound to evaluate blood flow through your veins, identifying any blockages or valve issues.
What is the Treatment for Varicose Veins?
A few varicose vein treatment options available as temporary or permanent treatments are:
- Compression stockings: These garments exert pressure on the legs, aiding blood circulation. They are available over the counter or as prescription strength, and insurance coverage may apply if symptoms are present.
- Varicose vein surgery procedures
- Sclerotherapy: Involves injecting a solution into varicose veins to close them. Multiple injections may be necessary, and the procedure can often be performed in the office without anaesthesia.
- Laser treatment: Uses bursts of light to fade varicose veins. It is a non-invasive procedure without cuts or needles.
- Catheter-based procedures (radiofrequency or laser energy): These methods involve heating and sealing varicose veins and are particularly effective for larger veins.
- High ligation and vein stripping: This outpatient procedure ties off and removes varicose veins through small incisions.
- Ambulatory phlebectomy: Smaller varicose veins are removed through tiny skin pricks, resulting in minimal scarring. This procedure is also performed on an outpatient basis.
What are the Complications/Side Effects of the Treatment?
Possible complications or side effects of varicose vein treatments include:
- Temporary bruising or discolouration in the treated area
- Swelling or discomfort may occur
- Skin irritation or rash could develop
- Allergic reactions to medications used during procedures are rare but possible
- Numbness or tingling sensations may be experienced
- Blood clots can occur, although they are uncommon
- Infection or nerve damage is rare, but potential risks
- Varicose veins may recur over time
- Scarring or changes in skin texture may occur
How Can I Prevent Varicose Veins?
Consider these lifestyle adjustments to potentially prevent varicose veins:
- Incorporate regular exercise to enhance blood flow and muscle tone. Aim for activities like walking or cycling for 30 minutes 3–5 times per week.
- Maintain a healthy weight to alleviate pressure on the veins.
- Adopt a balanced diet low in salt and rich in fibre to mitigate water retention, a factor contributing to varicose veins.
- Be mindful of your sitting posture; avoid crossing your legs and elevate your legs when seated or lying down.
- Opt for appropriate footwear, avoiding high heels or tight stockings except for compression stockings.
- Take breaks to change positions frequently, incorporating stretching or short walks every 30 minutes.
What is the Outlook for People with Varicose Veins?
The outlook for individuals with varicose veins is generally positive. With appropriate management, including lifestyle adjustments and medical interventions as necessary, most people can effectively control symptoms and minimise complications. However, regular monitoring is essential to prevent potential worsening or complications.
What are the complications of varicose veins?
- Ulcers: Painful sores may develop near varicose veins, particularly around the ankles.
- Blood clots: Enlarged veins deep within the legs can lead to clot formation.
- Bleeding: In rare instances, superficial veins may rupture.
- Leg swelling: Prolonged varicose veins can result in swelling of the legs.
Do varicose veins return after treatment?
Varicose veins can indeed recur after treatment, with approximately 60% of individuals experiencing a reappearance within five years.
When to see a doctor?
You should see a doctor if you notice persistent leg pain, heaviness, or swelling in your ankles or feet. Other concerning symptoms include skin discolouration around varicose veins, ulcers or sores near the affected area, sudden changes in the size or colour of the veins, or unexplained bleeding. These signs may indicate more serious issues, such as chronic venous insufficiency or infection. Don’t ignore these warning signals. Prompt medical attention can help diagnose the problem early, prevent complications, and ensure you receive the most effective treatment to manage your condition and improve your overall vascular health.
Conclusion
Varicose veins are common and can recur even after permanent varicose vein treatment. However, with proper management and lifestyle adjustments, individuals can often control varicose vein symptoms and minimise complications. Remember, regular monitoring is key to maintaining vein health. For convenient at-home testing and check-ups, consider using Metropolis Healthcare/Labs services, ensuring comprehensive care from the comfort of your home.
FAQs
How do I stop varicose veins from forming?
While you can't completely prevent varicose veins, several strategies can help lower your risk. Regular exercise improves circulation and strengthens muscle tone, which supports healthy blood flow. Maintaining a healthy weight reduces pressure on your veins, decreasing the likelihood of vein enlargement. Avoid prolonged periods of standing or sitting by taking frequent breaks to encourage movement and circulation. Elevating your legs when resting also promotes better blood flow. Additionally, wearing compression stockings provides extra support for your veins and can help prevent the development or worsening of varicose veins.
Will varicose veins go away?
Unfortunately, varicose veins generally do not disappear on their own. To eliminate varicose veins, treatments like sclerotherapy, laser therapy, or varicose veins surgery are needed to seal off or remove the problematic veins.
What drink is good for veins?
While no specific drink can cure varicose veins, staying hydrated is essential for maintaining healthy circulation. Aim to drink plenty of water throughout the day. Some studies suggest that flavonoid-rich drinks like tea and cocoa may support vein health, but more research is needed.
Can varicose veins be cured?
While there's no permanent cure for varicose veins, treatments can successfully manage the condition. Lifestyle modifications, compression therapy, and medical procedures can improve symptoms and prevent recurrence. However, varicose veins may reappear over time, especially if risk factors persist.
Is walking ok for varicose veins?
Yes, walking is highly beneficial for people with varicose veins. Regular walking promotes better blood circulation, alleviating symptoms and reducing the risk of complications. Aim for at least 30 minutes of brisk walking daily, gradually increasing your duration and intensity as tolerated.





1744887454.webp)



















